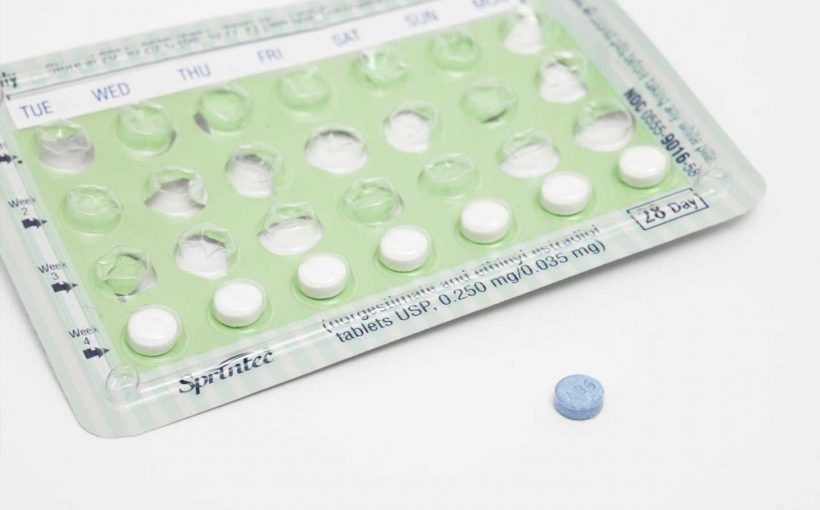
Across the United States, there are large differences in effective contraceptive use, according to a new study from Oregon Health & Science University, based on data from more than 8.5 million Medicaid beneficiaries.
The study was published today in the journal Health Affairs.
Medicaid covers the cost of contraception for millions of women across the country. Contraception is defined as a core benefit within Medicaid, but access and use vary substantially across the nation and within states, and there is little data to explain these differences. This is the first study to comprehensively assess how access to contraception for Medicaid beneficiaries varies based on where they live.
“States differ considerably in the services their Medicaid programs cover, and to whom care is provided, and this has significant implications on patients,” said lead author Maria Rodriguez, M.D., M.P.H., professor of obstetrics and gynecology in the OHSU School of Medicine and director of the Center for Reproductive Health Equity.
“Reproductive health is a fundamental right, yet so many Americans do not have equal access to care. I hope that the data revealed in this study will encourage providers and policymakers to address the gaps in our systems so we can improve the health of millions of women who are enrolled in Medicaid.”
In collaboration with OHSU’s Center for Health Systems Effectiveness, the analysis leveraged data from millions of Medicaid beneficiaries between the ages of 15 and 44. The sample included women living in nearly 3,000 counties across 40 states.
A multilevel analysis demonstrated substantial place-based inequities in both contraceptive use and access across the United States. Specifically, rates of effective contraceptive use—meaning taken as directed to prevent pregnancy—varied drastically between different counties, spanning a low of 10% to a high of 44%. The variation was even greater when looking at long-acting contraceptive options, such as intrauterine devices, or IUDs, and implants.
A variety of factors at the individual, state and federal level may contribute to these variations, including differences in state policies, provider networks and practices, individual preferences and pregnancy intentions, the influences of religious health systems and more.
Rodriguez notes that understanding these large geographical variations in contraceptive use may present opportunities for state and federal policies to improve reproductive health outcomes for millions of Medicaid beneficiaries. Recommended strategies include removing or loosening the control over which health care services are covered; incorporating quality metrics or value-based payments into contraceptive services; and adjusting reimbursements to remove barriers for providers of contraception.
Looking forward, Rodriguez warns that access to some forms of contraception may face growing restrictions, potentially widening the gaps identified in this study.
“Unfortunately, many of the legal efforts being made to restrict reproductive health care will only exacerbate these inequities,” Rodriguez said. “It’s crucial that we continue to fight for policies and practices that expand contraceptive access to ensure that all women—no matter where they live—can make informed decisions about their health.”
This study is a continuation of OHSU’s efforts to advance reproductive health services, education and policy research. OHSU is committed to providing the full continuum of sexual and reproductive health care to all who seek it.
More information:
Maria I. Rodriguez et al, Geographic Variation In Effective Contraceptive Use Among Medicaid Recipients In 2018, Health Affairs (2023). DOI: 10.1377/hlthaff.2022.00992
Journal information:
Health Affairs
Source: Read Full Article