A new study out this week in the journal Social Science and Medicine proposes that social, gendered variables may better explain observed sex disparities in adverse drug events than sex-based biology.
Adverse drug events refer to harmful side effects resulting from the use of a drug. A 1.5-2 times higher rate of adverse drug events in women compared to men has long been observed, and addressing this disparity has been an enduring priority of women’s health advocates, medical researchers, and institutions such as the National Institutes of Health.
Advocates and researchers have emphasized the need for more sex-based biological research to address this prominent sex disparity, and reducing adverse drug events in women was an explicit target of recent research policies introduced by the NIH requiring the study of sex as a biological variable in all preclinical research. However, critics of such policies point out that a primary focus on biological factors in driving these outcomes may be misplaced.
Using data from the U.S. Federal Adverse Events Reporting System (FAERS), a pair of papers published this fall by the Harvard GenderSci Lab reframes this debate by showing that:
- Accounting for underlying factors, such as baseline rates of medication use, greatly reduces the apparent sex disparity in adverse drug events. In a JAMA Open Network report, Rushovich, Gompers, and Lockhart et al. show that after incorporating baseline drug usage, the probability of a population sex disparity of 1.5-1.7—a magnitude claimed by many advocates of sex differences research—drops to less than 5%.
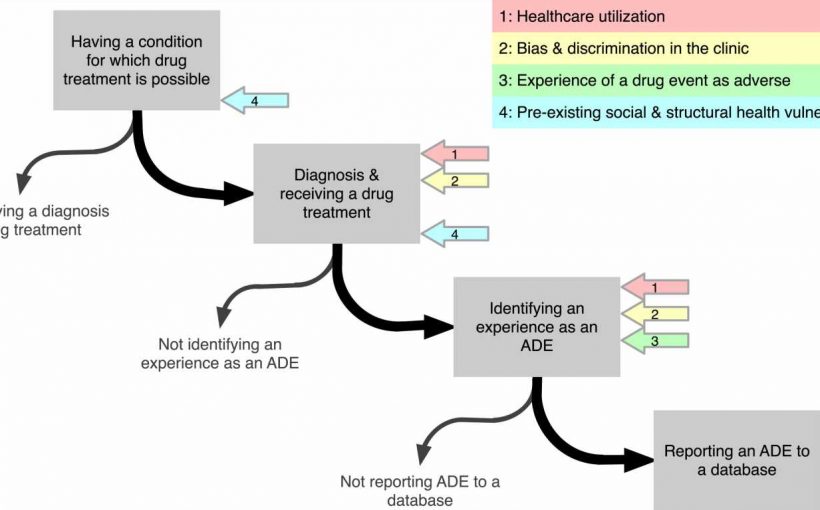
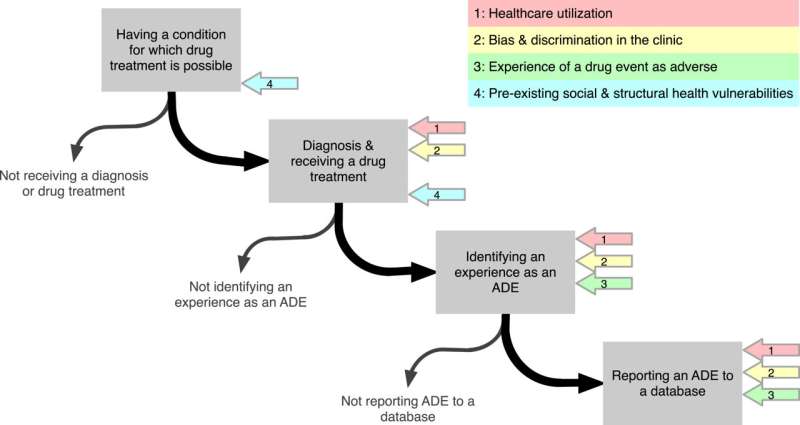
- The Gender Hypothesis proposes that health care utilization, bias and discrimination in the clinic, experiencing or perceiving an event as adverse, and upstream gendered social and structural determinants of health act as vital pathways by which gender shapes what may at first appear to be sex disparities in adverse drug events.
Dr. Katharine Lee, lead author of the Social Science and Medicine paper and assistant professor of anthropology at Tulane University, said, “Drug safety and adverse events are a commonly cited motivator for further research into biological sex differences. Our analyses show that gender—the social, structural, and experiential differences linked to individuals’ gender/sex identity across their lifetimes—is a powerful contributor to reports of adverse drug events and ultimately inequitable health outcomes.”
Dr. Sarah Richardson, Aramont Professor of the History of Science and of Studies of Women, Gender, and Sexuality at Harvard, and Director of the Harvard GenderSci Lab, said, “In these papers, we use data from over 33 million records of adverse drug events in large publicly available datasets to highlight that gender and related social factors, not simply biological sex, drive apparent sex disparities in adverse drug events.”
“The Gender Hypothesis generates predictions that can be tested in existing datasets and future study designs and identifies intervenable pathways driving sex disparities in ADEs.”
More information:
Katharine M.N. Lee et al, A Gender Hypothesis of sex disparities in adverse drug events, Social Science & Medicine (2023). DOI: 10.1016/j.socscimed.2023.116385
Tamara Rushovich et al, Adverse Drug Events by Sex After Adjusting for Baseline Rates of Drug Use, JAMA Network Open (2023). DOI: 10.1001/jamanetworkopen.2023.29074
Journal information:
Social Science and Medicine
,
Social Science & Medicine
,
JAMA Network Open
Source: Read Full Article