Researchers have discovered a new population of immune cells that are critical in maintaining the immune response against chronic infections and cancer. This population of T cells also mediates the response to immunotherapy using checkpoint inhibitors. The discovery may explain why immunotherapy fails in some people and could lead to the development of more effective new therapies for cancer or severe viral infections.
It has long been known that severe diseases can damage our immune system. Known as immune exhaustion, it is a phenomenon often seen in cancer patients or patients living with chronic viral infections such as HIV or hepatitis that mainly affects an immune cell population called cytotoxic T cells, which play a critical role by killing cancer cells or cells infected by a virus.
Now, a novel cell population that is critical in overcoming exhaustion and maintaining long-term T cell responses during chronic viral infection was identified by researchers, led by Dr. Veit Buchholz, a group leader at the Technical University of Munich’s Institute for Medical Microbiology, Immunology and Hygiene, and Prof. Axel Kallies, Laboratory Head at the Peter Doherty Institute for Infection and Immunity and the University of Melbourne.
Important results from previous studies
In previous studies, Veit Buchholz’s team had identified that certain memory T cell subsets had the stem-cell-like ability to self-renew, tracing immune responses derived from single T cells in vivo. In related research, Prof. Kallies’ team had demonstrated that not all T cells in chronic disease become exhausted and lose their function. So-called “precursors of exhausted T cells” or Tpex cells, were able to maintain their function for a long period of time.
‘A fountain of youth for T cell immunity’
The new study, published in Nature, combines the unique expertise of both labs, explains Dr. Carlson Tsui, a postdoctoral researcher in Professor Kallies’ laboratory and co-first author on the paper, narrowing it down to a very specific subset of Tpex cells that harbor this stem-cell-like function. “These cells are like the fountain of youth for T cell immunity, allowing exhausted T cells to self-renew and remain functional,” says Dr. Lorenz Kretschmer a postdoctoral researcher in Dr. Buchholz’s lab, and co-first author of the study.
Stem-like exhausted T cells maintain good immune response
“The success or failure of immunotherapy in cancer or chronic infection depends on the quality of the T cell response, and we have been able to pinpoint the precise subset of cells that is crucial in maintaining a good response,” says Veit Buchholz. The researchers have proposed this new subset of cells to be called stem-like exhausted T cells. “These cells act like stem-cells for the killer T cell population; they self-renew while also producing cytotoxic T cells that can kill virus infected cells,” Dr. Buchholz says.
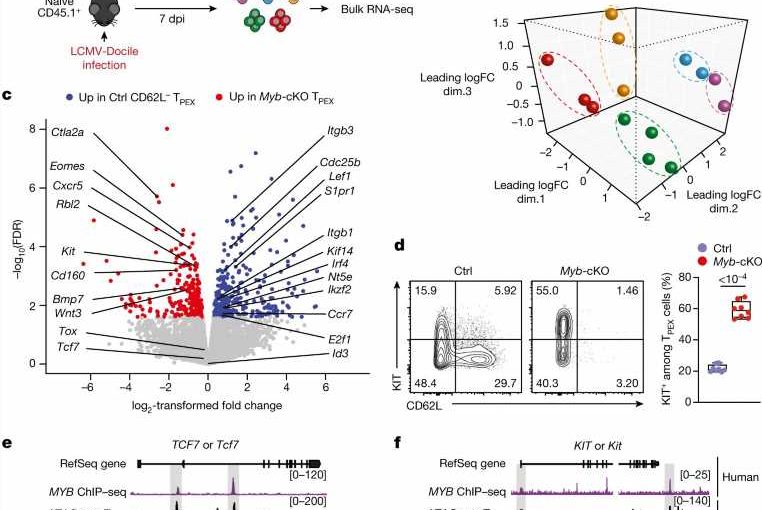
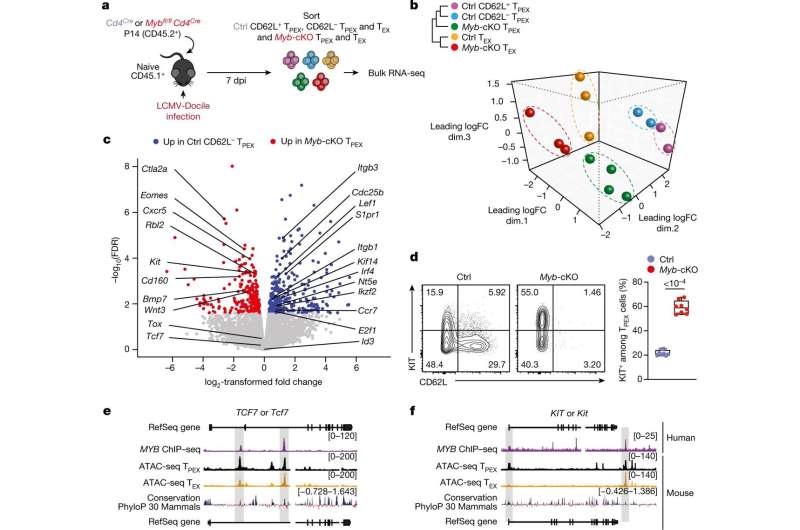
The team have also been able to identify the key molecule which enables these cells to develop and function. “We discovered a specific transcription factor, called Myb, that controls the development and function of these cells,” Prof. Kallies explains. “Without this factor, this population of cells doesn’t form, and the T cells responding to the chronic infection cannot be maintained or respond to checkpoint inhibition.” Immunotherapy using checkpoint inhibitors has been a crucial innovation for cancer therapy in recent years. “Basically, without this transcription factor, immunotherapy fails,” says Prof. Kallies.
Insights may lead to better targeted immunotherapies
Both teams are now working on new strategies to utilize these cells and are hopeful that their research will lead to better therapies. “Currently, immunotherapy is only successful in some cancers and only works for some patients,” Axel Kallies says.
Source: Read Full Article