New research from Boston Medical Center concluded that offering medications to treat opioid addiction in jails and prisons leads to a decrease in overdose deaths. Published in JAMA Network Open, the study also found that treating opioid addiction during incarceration is cost-effective in terms of healthcare costs, incarceration costs, and deaths avoided.
Overdoses kill more than 100,000 people per year in America and this number continues to increase every year. People with addiction are more likely to be incarcerated than treated, with those from communities of color who use drugs more likely to be incarcerated than white people.
Most prisons and jails in the United States discontinue medications for opioid use disorder (MOUD) upon incarceration, even if taken stably prior to incarceration, and do not initiate MOUD prior to release. Patients often suffer withdrawal symptoms while incarcerated and the post incarceration period is a time of very high-risk for overdose death.
“Offering medications for opioid addiction for incarcerated individuals saves lives. Specifically, offering all three medications—buprenorphine, methadone, and naltrexone—is the most effective at saving lives and is more cost-effective,” said lead author Avik Chatterjee, MD, primary care and addiction medicine physician at Boston Medical Center and Boston Healthcare for the Homeless and assistant professor of medicine at Boston University Chobanian & Avedisian School of Medicine.
“We hope our study supports policy change at the state and federal level, requiring treating opioid use disorder with medications among people who are incarcerated.”
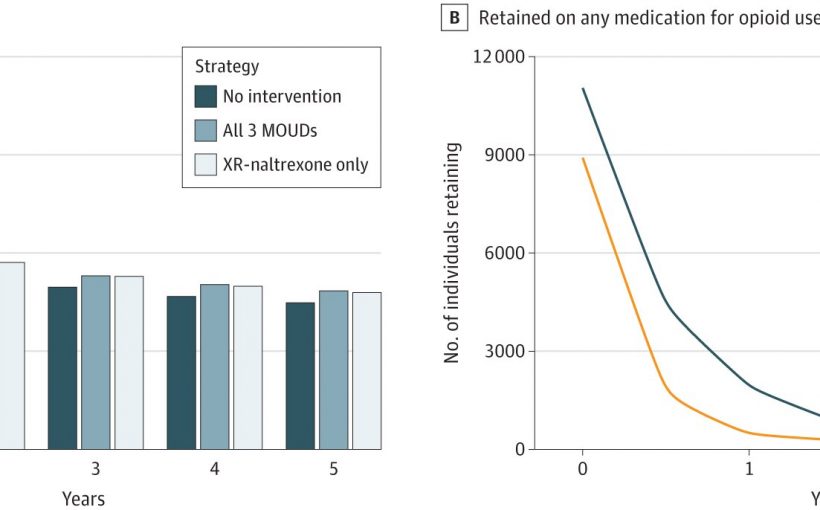
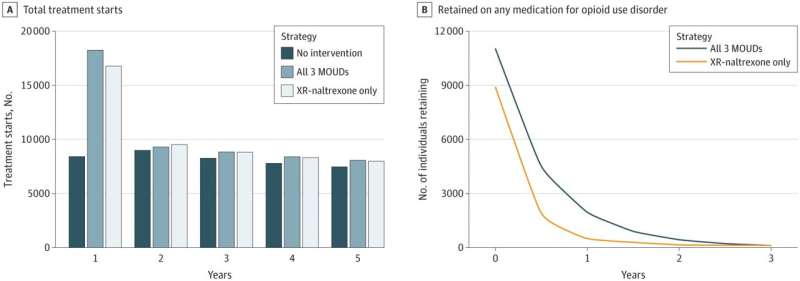
The study modeled the impact of MOUD access during and upon release from incarceration on population-level overdose mortality and OUD-related treatment costs in Massachusetts using three different strategies: 1) no MOUD provided during incarceration or upon release, 2) offer only extended-release naltrexone (XR-NTX) upon release from incarceration, and 3) offer all three MOUD at intake.
Among 30,000 incarcerated people with OUD, offering no MOUD was associated with 40,927 MOUD treatment starts over a 5-year period and 1,259 overdose deaths after 5 years. Over 5 years, offering XR-NTX at release led to 10,466 additional treatment starts and 40 fewer overdose deaths.
In comparison, offering all three MOUD at intake led to 11,923 additional treatment starts, compared to offering no MOUD, and 83 fewer overdose deaths. Among everyone with OUD in MA, “XR-NTX only” averted 95 overdose deaths over 5 years—a 0.9% decrease in state-level overdose mortality, while the all-MOUD strategy averted 192 overdose deaths—a 1.8% decrease.
In this simulation modeling study, researchers found that offering any MOUD to incarcerated individuals with OUD would prevent overdose deaths and offering all three MOUD would prevent more deaths and save money.
Researchers believe that a treatment-based approach is more appropriate than an incarceration-based one for treating addiction. Proactively offering treatment during incarceration can save lives and is a cost-effective health intervention, while also supporting the dignity of people who are incarcerated.
More information:
Avik Chatterjee et al, Estimated Costs and Outcomes Associated With Use and Nonuse of Medications for Opioid Use Disorder During Incarceration and at Release in Massachusetts, JAMA Network Open (2023). DOI: 10.1001/jamanetworkopen.2023.7036
Journal information:
JAMA Network Open
Source: Read Full Article